ICYMI: Updates to NCCI Edits Big Win for PTs
CMS National Correct Coding Initiative edits, known as NCCI edits, provide guidelines for what codes can be billed with evaluation codes and which modifiers may be required. As you can imagine, these rules can greatly impact reimbursement.
In January, CMS implemented strict changes about what could and could not be billed with an evaluation code. Since then, CMS has rescinded many of their changes in order to alleviate the significant burden that the update to the edits placed on providers during COVID-19.
PTS in both private practice and rehab agencies can pair many codes without adding the 59 or applicable X modifier. These changes are retroactive to January 1, 2020.
The Coding Changes
PTs are now able to pair the following code combinations without the use of 59 or X modifiers:
97530 with 97116
97161 with 97140
97162 with 97140
97163 with 97140
99281-99285 with 97161-97168
97110 with 97164
97112 with 97164
97113 with 97164
97116 with 97164
97140 with 97164
97150 with 97110
97150 with 97112
97150 with 97116
97150 with 97164
There are additional edit changes as well that can be viewed on the CMS links below.
Which Payers These NCCI Edit Changes Apply to:
Medicare and Medicaid follow CMS’ NCCI edits. Commercial payers also typically follow the edit guidelines but may not have updated yet based on the recent news. It is important to check with your insurance companies if you have denials come back for the previous edit guidelines.
Links to Learn More:
https://www.cms.gov/Medicare/Coding/NationalCorrectCodInitEd/Version_Update_Changes
LRS Webinar
Join Lincoln Reimbursement Solutions CEO, Bryanne Johnson, and President, Danielle Pantalone, for an interactive webinar on an in depth discussion of the Top 7 Billing Best Practices.
Now, more than ever, it is essential that you are collecting every penny that you are owed.
On the webinar, Bryanne and Danielle will walk you through the questions you should be asking your billing team on a quarterly basis to ensure your key metrics are being met and your bottom line isn't suffering unnecessarily.
Billing Best Practices
Below are some items you should be asking your billing team on a quarterly basis. These are your key performance indicators that directly affect your bottom line. If answers to these questions are drastically different quarter to quarter you will likely notice a difference in your cash flow.
What do my AR buckets look like?
• Is the 120+ less than 15% of the total AR?
What is my first pass payment percentage?
What is my Daily Sales Outstanding (DSO)?
What is my current payer mix?
What is my denial rate?
• What are my top 5 denial reasons?
• How many claims were written off in the last 90 days and what were the reasons for needing to write off?
What is the average reimbursement per visit for my top 5 insurance payers?
What are major insurance changes that I should be aware of?
• Who are my flat rate payers?
• Are any new insurances requiring authorization?
We are happy to talk through the answers you receive to these questions, review your contracts, and provide you with a strategic revenue analysis.
Save the Date For Our Billing Best Practices Webinar. Register here!
May 19th, 2020 @ 12:00pm EST
BREAKING NEWS: CMS Allows Therapy Providers to Deliver Telehealth
The moment we have been waiting for - CMS announced today that physical, occupational and speech therapy providers may deliver care via telemedicine for the duration of the COVID-19 pandemic.
This will allow clinicians to protect their most vulnerable patients and reduce the risk of spreading the virus. PTs, OTs and SLP can provide services to new or current Medicare patients.
Medicare will allow Physical and Occupational Therapy and SLP to provide the following services via telehealth. CPT codes 97161- 97168; CPT codes 97110, 97112, 97116, 97535, 97750, 97755, 97760, 97761, 92521- 92524, 92507. Please note that not all PT, OT and SLP CPT codes are currently allowed. See here for a comprehensive list.
As always, contact us with any questions. We will continue to monitor and share updates from CMS and other major commercial payers as they develop around telehealth.
Stay well!
Things You Should Know This Week
United Healthcare - New Guidance Sent Out This Week
To help you manage the claim submission and reimbursement process with UnitedHealthcare, as well as access the CARES ACT funding available to health care professionals, here’s a summary of resources to address your most common questions and concerns. Use this list of quick links as an easy reference to save you time.
Telehealth Coding Scenarios: This guide has helpful examples of how UnitedHealthcare might reimburse for telehealth services during the national emergency. UHC also released additional coding and reimbursement guidance available on their website.
Expanded Telehealth Access: Policies around telehealth have been expanded across all of our health plans.
Timely Filing: Claims with a date of service on or after Jan. 1, 2020 will not be denied for timely filing deadlines if submitted by June 30, 2020.
Videos to Help Guide Billing: Two videos are available for easy visual instruction on billing for COVID-19-related office visits and laboratory tests.
Prior Authorization Requirements: Many requirements have been suspended or eased during the national emergency period. Review specific details and dates here.
CARES Act Training: UnitedHealth Group has been selected to facilitate delivery of CARES Act Provider Relief funding through the U.S. Department of Health and Human Services (HHS). This user guide will help you navigate the HHS provider portal, and this quick tutorial outlines what you need to know to request or confirm additional relief funding.
Medicare
CMS announced that it is reevaluating the amounts that will be paid under its Accelerated Payment Program and suspending its Advance Payment Program to Part B suppliers effective immediately. The agency made this announcement following the successful payment of over $100 billion to healthcare providers and suppliers through these programs and in light of the $175 billion recently appropriated for healthcare provider relief payments.
For more information on the CARES Act Provider Relief Fund and how to apply, visit here.
For an updated fact sheet on the Accelerated and Advance Payment Programs, visit here.
States Resuming Elective Surgeries
Becker’s Healthcare is keeping a running list of states as they announce plans to resume elective surgeries. Is your state on here? Bookmark the list here.
Paycheck Protection Program Updates
An SBA loan that helps businesses keep their workforce employed during the Coronavirus crisis has resumed as of April 27, 2020. The SBA has started accepting Paycheck Program applications from participating lenders. If you're a small business, look into applying here or contact your local bank.
Sharpen Your Axe with LRS!
Sharpen Your Axe with LRS!
““Give me six hours to chop down a tree and I will spend the first four hours sharpening the axe.” - Abraham Lincoln”
At LRS, we pride ourselves on implementation and improvement. Our company is named after Abraham Lincoln - we focus on ways to make your practice more efficient and in turn, collect every penny of what you are owed.
Since we started our company six years ago, we have been sharpening our axes. Here are several of the ways we can help you:
LRS works as a clearinghouse to reduce the administrative burden that is placed on the medical practice and instead allows you to focus on providing quality care to your patients.
Now, more than ever, it is essential that you collect on every claim you have outstanding. Let us help you attack your AR and clean up any outstanding debts you have.
Insurance Verifications & Authorizations
We understand that you may be working with a lean staff right now. We can take over verifications and authorizations for you to ensure the patients that you are seeing are going to be covered for service.
Now is a great time to make a switch for your full revenue cycle management. We will guide you through the process every step of the way and hit the ground running submitting your claims, working your denials and AR, and collecting every penny you are owed.
Things You Should Know This Week
Accelerated Payments
CMS released information on the expansion of its accelerated and advance payment program for Medicare participating health care providers and suppliers, to ensure they have the resources needed to combat the 2019 Novel Coronavirus (COVID-19).
A Medicare provider/supplier who submits a request to the appropriate Medicare Administrative Contractor (MAC) and meets the required qualifications will be able to request up to 100% of the Medicare payment amount for a three-month period. Review of the accelerated/advanced payments are handled by the providers and suppliers’ MAC. Electronic submission is preferred and MACs are supposed to review the submission within seven calendar days of the request. The provider/supplier can continue to submit claims as usual after the issuance of the accelerated or advance payment; however, recoupment will not begin for 120 days.
Learn more on the CMS fact sheet here.
Also, CMS isn’t the only insurance provider who is offering accelerated payments. Check with your billing team to see if your other major payers have this as an option.
Telehealth Relief Application
The COVID-19 Telehealth Program will provide $200 million in funding, appropriated by Congress as part of the Coronavirus Aid, Relief, and Economic Security (CARES) Act, to help health care providers provide connected care services to patients at their homes or mobile locations in response to the novel Coronavirus 2019 disease (COVID-19) pandemic.
On April 2, 2020, the Commission released an order establishing the COVID-19 Telehealth Program. The COVID-19 Telehealth Program will provide immediate support to eligible health care providers responding to the COVID-19 pandemic by fully funding their telecommunications services, information services, and devices necessary to provide critical connected care services until the program’s funds have been expended or the COVID-19 pandemic has ended.
Stimulus Relief Fund Payment
Approximately $30 billion in payments was distributed to Medicare Part B providers in proportion to their overall share of Medicare Fee for Services payments that were made to the participant during 2019. Providers were distributed a portion of the $30 billion based on their share of total Medicare FFS reimbursements in 2019.
However, there are strings attached to these CARES Act Provider Relief Funds. Please see here for the applicable payment terms to consider before using any of the funds.
THANK YOU!
We wanted to take a moment to thank all of you health heroes. In the wake of our new reality of ‘flatten the curve,’ where social distancing and face masks are the new norm and quarantine measures are widely practiced, you all are still showing up every day for your patients. So many of you have stepped up in incredible ways - transitioning to telehealth models quite literally overnight, ensuring your clients (and clinicians) safety in your offices, and continuing to provide the highest levels of care to the communities and vulnerable patients you serve.
A quote from Theodore Rubin has resonated with us during this time:
Happiness does not come from doing easy work, but from the afterglow of satisfaction that comes after the achievement of a difficult task that demanded our best.
The pandemic has demanded our best. We will get through it together.
Thank you for all you do.
With admiration,
Bryanne and Danielle
Using This Time to Clean-Up Your A/R
Using This Time to Clean-Up Your A/R
In the midst of this chaos (and most likely as you are seeing less patients), it is more important than ever to collect every penny you are owed.
The best way to do this is to start a complete A/R overhaul.
At LRS, we are A/R clean-up professionals!
A few details on how we attack your outstanding claims and get you paid faster:
We review each and every individual claim that is aged out over 90 days.
We handle all the rebilling, recommendation of write offs, correcting of claims, appealing of denials, and anything else that may need to be done to bring the claim to a resolution.
We provide you with a spreadsheet with each of these claims with the reason they are outstanding and what the anticipated outcome is for each claim so you know exactly how much money you can expect to be coming in the door.
As always, through this A/R process and through everything we do at LRS, we really pride ourselves on our communication with your entire team.
Do you want to learn more about how we could help? Contact bjohnson@lincolnrs.com to set up a time to talk.
Insurance Updates to Implement This Week
Several announcements have been made regarding policies during COVID-19.
CMS has temporarily halted sequestration under Medicare. Starting on May 1, 2020 and extending through December 31st, 2020, CMS will no longer sequester 2% from allowable Medicare payments.
UnitedHealthcare has approved telehealth for therapy providers. This is subject to state laws and regulations around telehealth, but, if permissible, this enables physical therapists, occupational therapists, and speech therapists to provide true telehealth services. Eligible codes will be reimbursed by UHC with a place-of-service code 02 and the 95 modifier.
CIGNA has created telehealth policies for therapy providers. These measures allow for reimbursement of PT services that include codes 97161 (evaluation, low complexity, 20 minutes, telephone or virtual), 97162 (evaluation, moderate complexity, 30 minutes, virtual), and 97110 (therapeutic exercises, two unit limit). Codes must be appended with a GQ modifier and billed with a standard place-of-service code.
Each payer is providing different guidance on how to bill for telehealth services so it is important that they are set up correctly in your EMR system.
If you have any questions about billing for telehealth services (or getting set up to provide it), please don’t hesitate to contact us. We are here to help.
COVID-19 and Industry Updates
We hope you are staying well during this time. We wanted to highlight a few news updates both COVID-19 related and industry news related.
As a reminder, Contact your legislators today and ask them to pass The Creating Opportunities Now for Necessary and Effective Care Technologies (CONNECT) for Health Act (HR 4932/S. 2741). This is bipartisan legislation that would expand the use of telehealth services and ease restrictions on telehealth coverage under the Medicare program. Click here to send a letter directly to your Congressional Members.
In other news, TRICARE has issued the final rule to add PTAs and OTAs as TRICARE authorized providers for PT or OT services under the supervision of a TRICARE-authorized PT or OT in accordance with Medicare’s rules for supervision and qualification. General supervision requires the PT or OT to be available if needed by the PTA or OTA but does not require the PT or OT to be in the office suite or on the premises. Tricare may still implement CQ and CO modifiers. This will be effective April 16, 2020. Read more about the final rule from the GAO.
As a reminder, AIM auths are scheduled to go-live on 04/01/2020 for the following plans:
Anthem Medicaid IN, NY, WI
Anthem Commercial CO, NV
Anthem Medicare CA, CO, CT, GA, IN, KY, ME, MO, NH, NM, NY, OH, TN, TX, VA, WA, WI.
For services that are scheduled on or after 04/01/2020, providers must use AIM to obtain authorization for outpatient rehabilitation services. The online portal can be used 24/7 to place authorization requests, and many times, the determination is made at the time of submission! Visit here to register today!
As always, we are here to help. Be well.
Click here to read how we’ve taken our security more seriously in this article with our President and Co-Founder, Danielle Pantalone and Paobox!
We Are Here To Help
Here To Help
Telehealth, E Visits, Reimbursement and More…
We know this is an extremely difficult time to be a business owner and that each day brings new challenges for you and your clinics.
Now more than ever, it is important to focus on your Revenue Cycle and clean up your AR and make sure you are collecting every penny that you've earned.
If you are continuing to see patients in the clinic and/or via telehealth, we can assist getting you set up with your payers and also with billing out your current claims to ensure payment as quickly as possible.
We want to be a resource in any way that we can. Let's band together and continue to operate in one of the best communities in healthcare. We are here to help.
Transitioning to Teletherapy
Transitioning to Teletherapy
Information, interpretations and opinions seem to be falling from the sky regarding Medicare, teletherapy, e-visits, reimbursement and when and how these visits should be billed.
We are currently assisting our partners through the transition to teletherapy and we are here to help you too.
If you would like to schedule a call to discuss teletherapy and your practice, please contact us today.
COVID-19 and Part B Updates
CMS has released additional guidance on COVID-19 and Medicare Part B. You can read more here.
Here are a few important additional updates:
Medicare Advantage plans may provide their enrollees with access to Medicare Part B services via telehealth in any geographic area and from a variety of places, including beneficiaries’ homes. Medicare Advantage Organizations can expand coverage of telehealth services beyond those approved by CMS.
It is essential to verify with all insurances ahead of time whether or not they cover telehealth. If an insurance company says they will not cover telehealth, you can choose to see the patient via telehealth and appeal if the visit does end up being denied. This is a fluid situation and the insurance company is likely updating their policies in real-time. You can also offer patients self-pay for telehealth services.
The Coronavirus-19 Emergency Declaration Health Care Providers Fact Sheet lists multiple waivers that will help providers see patients in a more efficient and timely manner. This temporarily waives requirements for out of state providers to see patients and postpones revalidation requirements. You can read more here.
We will do our best to provide any updates from CMS and commercial insurance companies as they are released. The safety and health of your patients and of your teams is our main concern and we will continue to be in communication as this situation moves forward.
COVID-19 and Telemedicine
We have had several of our partners reach out to us to ask about the possibility of providing telehealth as Coronavirus continues to spread across the country.
The answer to that question is extremely complicated and fluid.
Many practices have already instituted telemedicine to help eliminate barriers to care for patients. However, not every insurance payer is willing to cover these telehealth visits.
As of this moment, telehealth is NOT a widely covered benefit under the Medicare fee schedule. Each commercial payer has different regulations and fee schedules regarding reimbursement and telemedicine and these regulations differ by each state. Each state’s practice act may also have restrictions on whether or not you can provide telehealth.
If you are inquiring with your top payers about telemedicine, let them know where your originating site will be (home or office) to verify whether it will be covered. There may be additional questions and restrictions regarding the care you can provide via telemedicine.
We will continue to keep you updated on if CMS temporarily changes course to include specific specialties as a covered telemedicine benefit and on any other payer news regarding telemedicine. As always, we are here for you as a resource and are happy to answer any questions you may have on this topic.
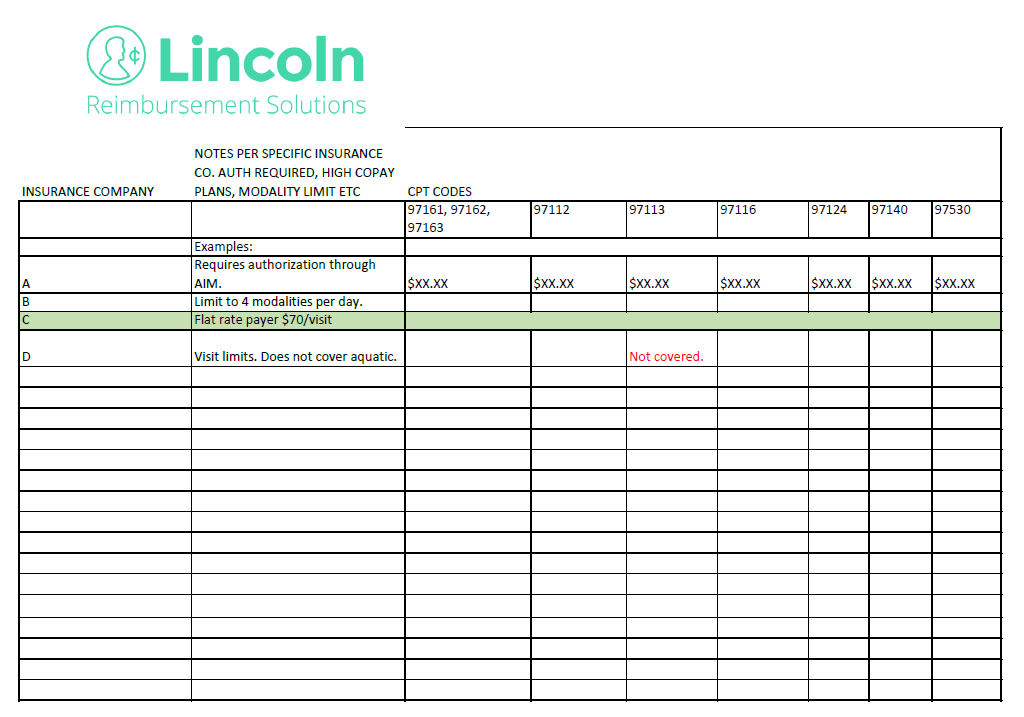
Downloadable Payer Cheat Sheet Template
Insurance companies are constantly updating, altering, reversing, swerving and dodging paying you in any and all ways that they can!
Your billing team plays a pivotal role in addressing these challenges and alerting the leadership team to what they are seeing on insurance payment EOBs.
To help assist you and your team, we created a Payer Cheat Sheet that your billing team can complete for your practice. Your clinical team can then use this cheat sheet to adjust payer and billing guidelines in your EMR to ensure you are optimizing your coding.
This file is best created in Excel. Contact us at hello@lincolnrs.com and we share the template and/or help get you started!
Is Your Prior Authorization Process Up to Speed?
Insurance companies are not going to stop requiring prior authorization. In fact, insurance companies are increasing their prior auth requirements including Anthem Blue Cross Blue Shield and United Healthcare.
New Prior Auth Requirements for Anthem Blue Cross Blue Shield
We are seeing several commercial plans across the country implement strict prior authorization requirements. We wanted to share a few examples of specific plans but even if these plans haven’t changed requirements in your state yet, you can bet these or other plans will be implementing similar requirements as the year goes on. Effective November 1, 2019, Anthem Blue Cross patients in over a dozen states require prior authorization to receive outpatient physical, occupational and speech therapy services. The initial evaluation does not require prior authorization, but treatment provided on the same date of service as the initial evaluation may require prior authorization depending on the payer rules.
This new program is being overseen by AIM Specialty Health. AIM’s Rehabilitation Program provides a clinical appropriateness review process that encompasses the duration of rehabilitation services. The program includes review of rehabilitative and habilitative outpatient physical, occupational and speech therapy services for medical necessity. The AIM Rehabilitative program for Anthem’s Commercial Membership will relaunch April 1, 2020 for Colorado and Nevada. The AIM Rehabilitative program for Anthem’s Medicare Advantage membership will launch April 1, 2020 for: California, Colorado, Connecticut, Georgia, Indiana, Kentucky, Maine, Missouri, New Hampshire, New York, Ohio, Tennessee, Texas, Virginia, Washington, Wisconsin and Texas.
New Prior Auth Requirements for United Healthcare
Similarly to Anthem, UnitedHealthcare Community Plan has announced they will implement prior authorization for outpatient physical, occupational and speech therapy services in select states. This process has already begun in many states. In addition, UnitedHealthcare Community Plan has announced they will be conducting site of service medical necessity reviews for all speech, occupational and physical therapy services in select states. For some states, the member’s referring physician will be required to submit prior authorization requests for evaluations and re-evaluations.
Once the physician has submitted the request for an evaluation or reevaluation and the request has been approved, the therapy provider can then request therapy visits. In the past, the prior authorization requests were submitted by the therapy provider. If UnitedHealthcare Community Plan does not have the authorization on file prior to the initiation of therapy services, therapy services will be denied and the provider will be unable to balance bill the patient. Additional prior authorization requirements are coming for UHC MyCare plans later this year.
What Can You Do About New Prior Auth Requirements?
Verifying a patient’s insurance is essential. By verifying a patient’s insurance prior to their appointment, you can estimate their patient responsibility, provide them visit limits, and know if their plan requires prior authorization or authorization. These requirements can be a lot for a front desk staff person to handle. LRS can help reduce these significant administrative burdens by taking on your verifications and authorizations so that your front desk can focus on the customer service experience for patients in your facility. Want to learn more about how LRS can assist in your verification and authorization process? Reach out to hello@lincolnrs.com and we can set up a time to chat!
Come Visit LRS at CSM!
The APTA CSM conference in Denver is almost here! If you or anyone in your organization are planning on attending, be sure to swing by Booth #2324 to say hello and find out how LRS might help to increase your revenue and decrease your administrative headaches!
Here are the exhibit hall hours for your reference:
Thursday, February 13th, 9:30 AM - 4:00 PM
Friday, February 14th, 9:30 - 4:00 PM ♥️
Saturday, February 15th, 9:30 AM - 3:00 PM
Interested in having coffee or a drink with us while at CSM? Email bjohnson@lincolnrs.com to set up a time!
Is Your EMR in Transition? 6 Tips to Help You Navigate
There have been so many changes in the physical therapy EMR world over the last few months - mergers, acquisitions, and overall instability when it comes to knowing who is managing your billing software.
We know the transition of an EMR can bring dread to you and your team. Luckily, LRS is here to help you navigate these transitions and ensure your revenue stream experiences no delays.
Here are 6 tips to help you survive (and thrive!) through an EMR transition:
Identify Existing Operational Issues: You want to start clean in your new system. If you are receiving denials for not verifying patient insurance correctly and subsequently missing authorizations, those same issues will carry over to a new system. Now is the chance to make sure all of your up-front processes are in place so you can be set up for success in your new EMR.
Allow Yourself Enough Time: Make sure you and your whole team take all available trainings in the new system, are practicing getting acquainted with flow of the software, and that you move your schedule and caseload over from your current software prior to your go-live date. You also want to make sure your billing partner is ensuring all billing rules, fee schedules, modifiers, etc. are set up correctly in the new system.
Plan for Your Old A/R: Who is going to work the claims in your old EMR system? If you have an in-house biller, this is self explanatory but ensure that you have access to the old EMR system for long enough to continue to work claims. If you are switching to a new billing company, what is your contract with the old system? Who owns the ability to work that A/R? Have these conversations early to avoid confusion down the line.
COMMUNICATE!: This cannot be overstated. Communicate with your old software support team, new software support team, your internal operational team, your billing team, your clinical team - integrate and communicate at all levels to ensure each team member has what they need to successfully complete their duties in the new system.
Monitor Your KPIs: Before you transition, identify your Key Performance Indicators. These should be first pass payment rates, revenue/visit, and other key metrics for your practice. Monitor these during the transition to ensure all essential KPI numbers are being met.
Focus on the Patient, Not the Computer: Above all, patient care comes first. Allow your billing partner, like LRS, to help you navigate the transition so you can do what you do best - take care of your patients.
Thinking about transitioning your software? Contact hello@lincolnrs.com to learn how LRS can help support you through the change.
Are You Attending CSM 2020?
The APTA Combined Sections Meeting is being held next month in Denver.
LRS will be there! Will you?
We would love to have the chance to buy you a cup of coffee and chat about how we might be able to help improve your revenue cycle. If you plan on attending, let us know by filling out the below form and we will contact you to set up a time to meet.